
What is it?
Ankylosing spondylitis (AS) is a type of arthritis, which mainly affects the bones, muscles and ligaments of the spine. It can also be found in other joints of different parts of the body.
The literal definition is ankylosis, meaning fusing, spondy- meaning spine, and –itis meaning inflammation.
AS, as most types of arthritis, causes inflammation and pain in the affected joints and tissues. Sacroiliac joints are mainly affected. Male individuals between 15-35 years of age are of a higher risk at developing the disease. The cause is unknown, although there is a strong genetic tendency.
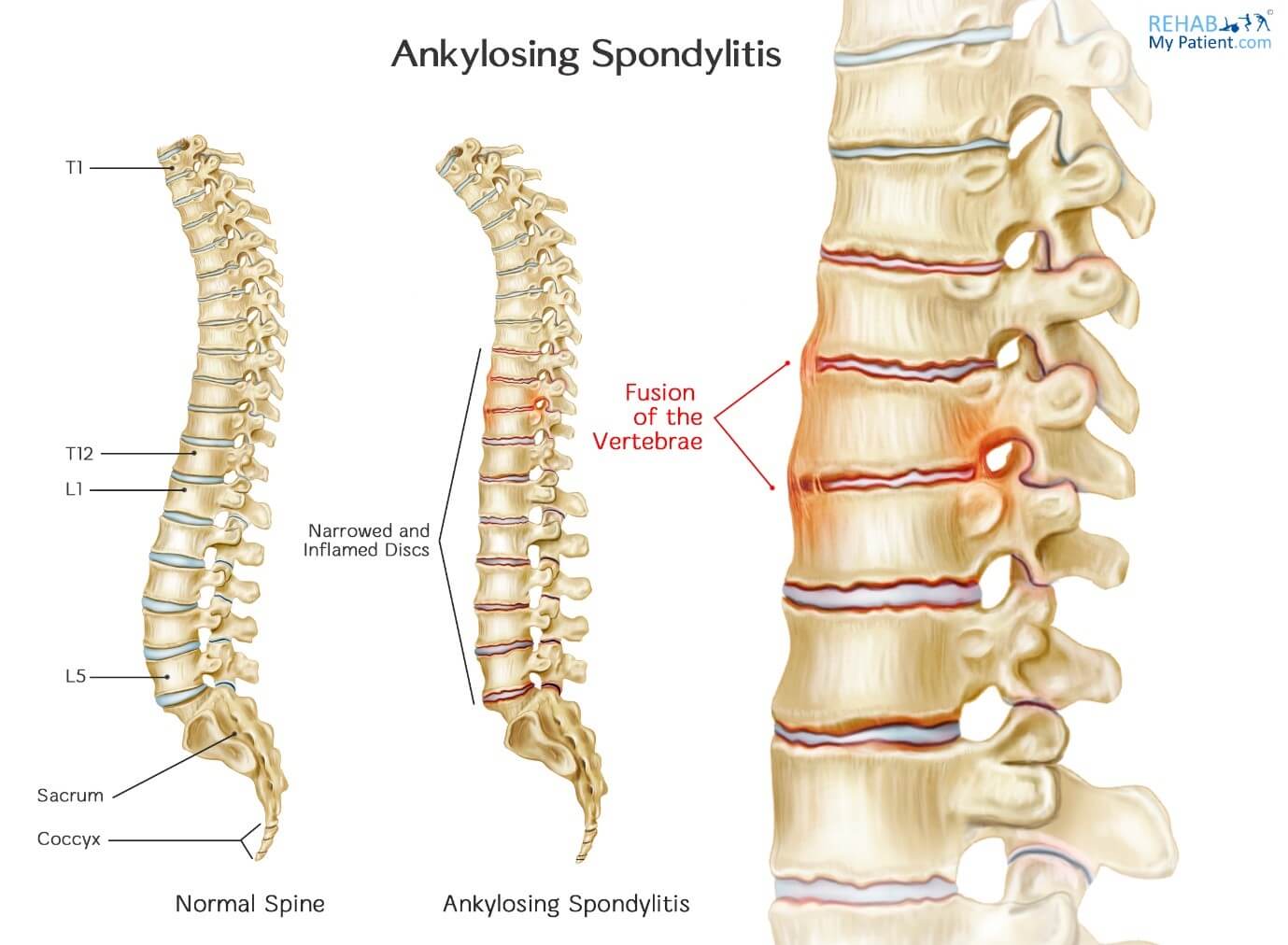
The inflammation process in AS can be quite destructive to the spine. It affects the facet joints (joints between each vertebra), and discs. It causes degenerative diseases in the spine and this leads to fusion of the joints. The body reacts to this by forward flexing (bending forwards) and after a few years sufferers can be quite disabled due to the forward bending in the spine.
AS can also affect other organs, like the heart, eyes, bowels and lungs. But this depends on the severity of the AS. Like many conditions, AS can affect a person mildly or severely and any range in between.
Signs & Symptoms
- Low back pain that gradually becomes worse and associated buttock pain
- Rest does not relieve pain
- Stiffness in the lumbar spine that is worse in the morning (lasts for more than 30 minutes), and eases throughout the day
- Pain and tenderness over the affected joints
- Swelling and increased temperature in the affected areas
- If rib joints are affected, chest pain and difficulty breathing may be present
- General symptoms such as: fatigue, depression, weight loss or anaemia
If you suspect you have AS, first discuss this with your therapist or doctor. Your doctor might refer you to a rheumatologist who will investigate and diagnose your condition.
AS may be diagnosed initially by MRI scan and confirmed by blood tests. A very specific blood test is required called an HLA-B27. This stands for human leukocyte antigen and its presence is often associated with AS and other inflammatory diseases. However, it is possible to have the HLA gene in the body, but not necessarily be symptomatic.
Treatment
Treatment options aim at relieving symptoms and delay the stiffening process, as there is no cure.
- Physiotherapy/Osteopathy/Chiropractic: a therapist can set up a suitable exercise programme with the most effective exercises for your complaints. Massage, hydrotherapy and electrotherapy are commonly used to relieve pain and promote mobility and flexibility.
- Medication (painkillers, corticosteroids, biphosphonates).
- Medication – discuss this with your doctor. Initially anti-inflammatory medication may be used. After this, steroids might be used such as prednisolone. Other forms of medication might also be used like Anti-TNF medication (examples: typically they end in –umab like adalimumab, or golimumab). There are also DMARDs (disease-modifying anti-rheumatic drugs).
- Exercises and a home exercise programme: keeping active is key. Your therapist will prescribe exercises to stop you forward bending your spine, and to extend your spine instead to help keep your back straighter. General exercises that are very useful include swimming and walking.
- Surgery is very rarely performed, and can be very complicated and exhaustive due to the multi-level degenerative changes affecting a larger area of the spine.
Tips
- Maintain physical activity is essential to manage stiffness (swimming and walking are suitable low-impact exercises).
- Maintain good posture.
- Lie flat (either on your back or abdomen) for at least 10 minutes per day.
- A hot shower in the morning can reduce stiffness whereas ice packs can sooth inflammation.
- Take regular breaks at work to stretch your body.
- Stop smoking as it may cause difficulty breathing.
Sign Up
Sign up for your free trial now!
Get started with Rehab My Patient today and revolutionize your exercise prescription process for effective rehabilitation.
Start Your 14-Day Free Trial