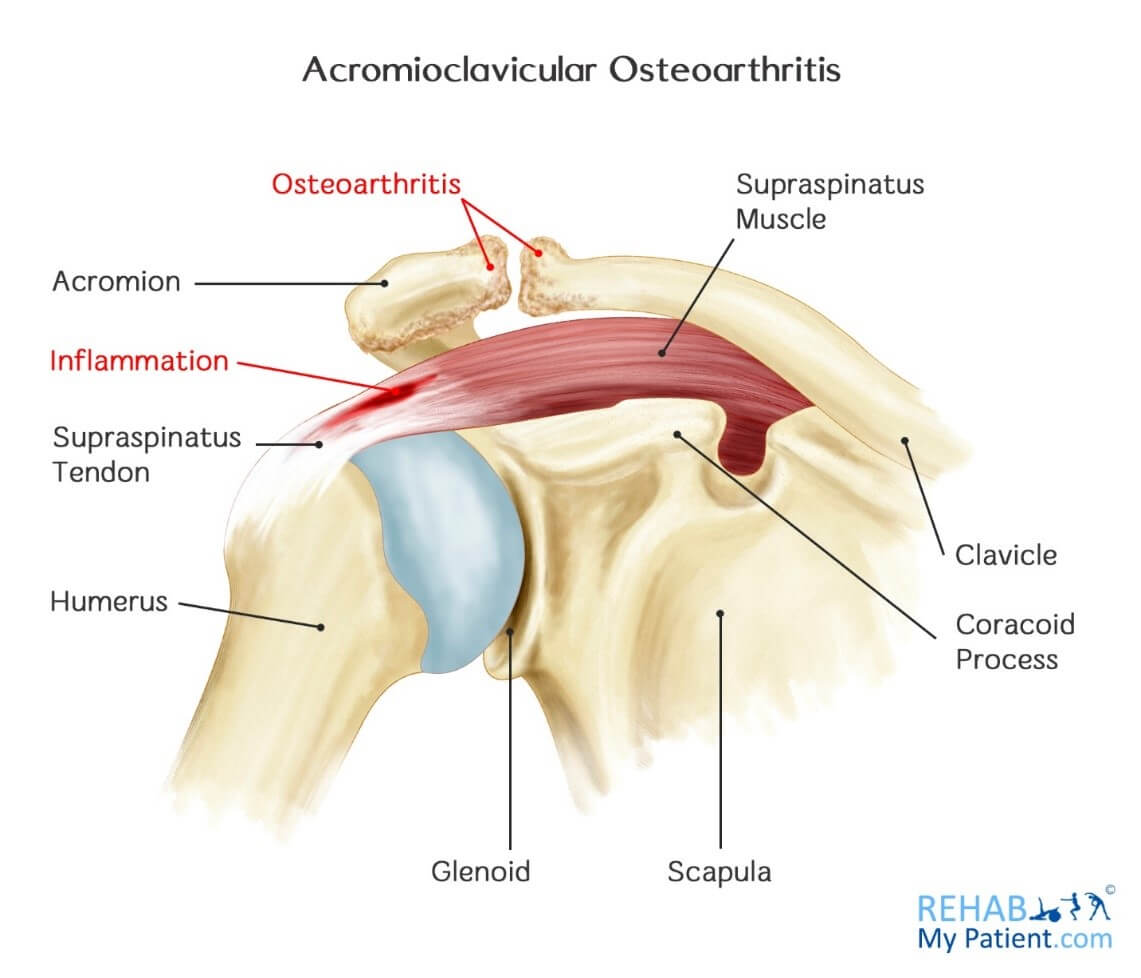
The acromioclavicular joint (known as the AC joint, or ACJ) is the joint between the clavicle (collar bone) and the acromion (the top of the shoulder blade). The ends of the bones are covered in cartilage, and when the cartilage wears out, degeneration (arthritis) can occur.
Most ACJ arthritis is caused simply by wear and tear of the joint over several decades. Hence the risk of developing osteoarthritis in the shoulder, as well as physical limitations and pain, increases as you grow older. Typically people with manual jobs or laboring jobs are at risk, as are weight-lifters and sports people (tennis, rugby, boxing are all common).
An injury, such as that of a dislocated shoulder, can end up leading to arthritis in the shoulder, regardless of how old you are. This is attributed to swelling, pain and even the development of bone spurs, whenever the two bones are rubbing together.
Most of the time, the condition occurs in those who are over the age of 50. In younger individuals, the condition can result from trauma or injury, such as a dislocated shoulder or a fractured shoulder, which is known as posttraumatic arthritis. The condition can also be hereditary.
Acromioclavicular Osteoarthritis Anatomy
The shoulder is composed of two joints, the glenohumeral joint and the acromioclavicular joint. The AC joint is where the collarbone joins the acromion, which is at the tip of the shoulder blade. The glenohumeral joint is where the top part of the arm bone meets the shoulder blade. Osteoarthritis is often found within the acromioclavicular joint.
ACJ arthritis can lead to other problems, the most common being shoulder impingement. The arthritic joint typically gets larger, or what we call hypertrophies. Bone spurs can also form under the joint. This can impinge the rotator cuff tendon that sits under the joint and this impingement can be very painful and lead to gross restriction in arm movement.
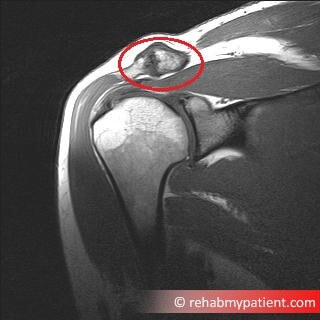
An MRI scan showing osteoarthritis of the AC Joint
On the above MRI scan you can see how the AC joint looks enlarged, thickened, and rough. You will also see the underlying muscle (at the bottom of the red circle) which is the supraspinatus muscle and tendon, deviating away from the ACJ due to shoulder impingement.
How to Treat Acromioclavicular Osteoarthritis:
1. Gentle movement, but try to avoid pain
The individual with arthritis needs to change the manner in which they are able to move the arm when performing regular daily activities in life. Someone who wears clothes that go over the head might need to wear those that zip up the front. Propping up hairdryers might be required instead of trying to hold onto them for the duration of the drying process.
2. Anti-Inflammatory Medication
Taking an anti-inflammatory medication can help to reduce pain and inflammation. Discuss with our doctor as it may not be a long term solution.
3. Physical Therapy
Manual therapy is however a long term solution, as the therapist can improve the mobility of the joint and offload stress to it, as well as working on your posture that can predispose this condition. Working with a physical therapist can help to strengthen the joints and muscles within the injured area.
4. Range-of-Motion Exercises
Performing specific exercises can help to increase flexibility and movement in the joint.
5. Ice
Apply ice to the shoulder for five to 10 minutes at a time, three to five times per day. The ice works to reduce pain and inflammation in the joint.

6. Dietary Supplements
Many individuals claim to find relief taking dietary supplements like chondroitin and glucosamine. Even though the evidence is conflicting on the use of supplements, you want to discuss these with your doctor because they might interact with other drugs.
Tips:
1. Most of the time, osteoarthritis is related to aging. When it comes to aging, the water content in cartilage increases and the protein makeup of the cartilage ends up degenerating.
2. Repeatedly using the joints over the course of years will cause damage to the cartilage leading the swelling and joint pain.
3. Since the condition can be found in multiple family members, it is often implied as a hereditary condition.
4. The condition might be the direct result of a defect in the collagen, which is an integral component of cartilage.
5. Growth hormone disorders and diabetes are often attributed to early wear of the cartilage and osteoarthritis.
Sign Up
Sign up for your free trial now!
Get started with Rehab My Patient today and revolutionize your exercise prescription process for effective rehabilitation.
Start Your 14-Day Free Trial